Canker Sores: What You Need to Know
Canker sores, also known as aphthous stomatitis, are painful ulcers that develop on the soft tissues of the mouth, including the inner cheeks, tongue, lips, and gum base. They are more common in younger individuals, and while often harmless, recurrent cases should not be ignored as they may indicate an underlying health condition. It is also crucial to differentiate them from other similar-looking lesions like herpes simplex ulcers, shingles (herpes zoster), acute necrotizing ulcerative gingivitis (ANUG), or erythema multiforme, as these may be associated with serious systemic conditions such as immunodeficiency, leukemia, diabetes, or nutritional deficiencies.
This article explores the causes, symptoms, diagnosis, treatment, and prevention of canker sores, along with when to seek medical attention.
What Are Canker Sores?
Canker sores are round or oval ulcers with a white or yellowish center surrounded by a red border. They typically cause pain, discomfort, and a burning sensation before appearing. Unlike cold sores, canker sores are not contagious and do not appear on the lips.
Common Causes and Risk Factors
The exact cause of canker sores is unknown, but several factors contribute to their occurrence:
- Oral Trauma: Accidental cheek biting, aggressive tooth brushing, dental appliances like braces, or poorly fitting dentures.
- Stress and Hormonal Changes: Emotional stress and hormonal fluctuations, such as those occurring during menstruation.
- Nutritional Deficiencies: Deficiency in vitamin B12, iron, folic acid, or zinc.
- Food Sensitivities: Spicy, acidic, or citrus-based foods can trigger or aggravate canker sores.
- Underlying Systemic Conditions: Conditions like celiac disease, Crohn’s disease, Behçet’s disease, and HIV/AIDS.
- Medications: Some medications, including certain pain relievers, beta-blockers, and chemotherapy drugs, may trigger recurrent ulcers.
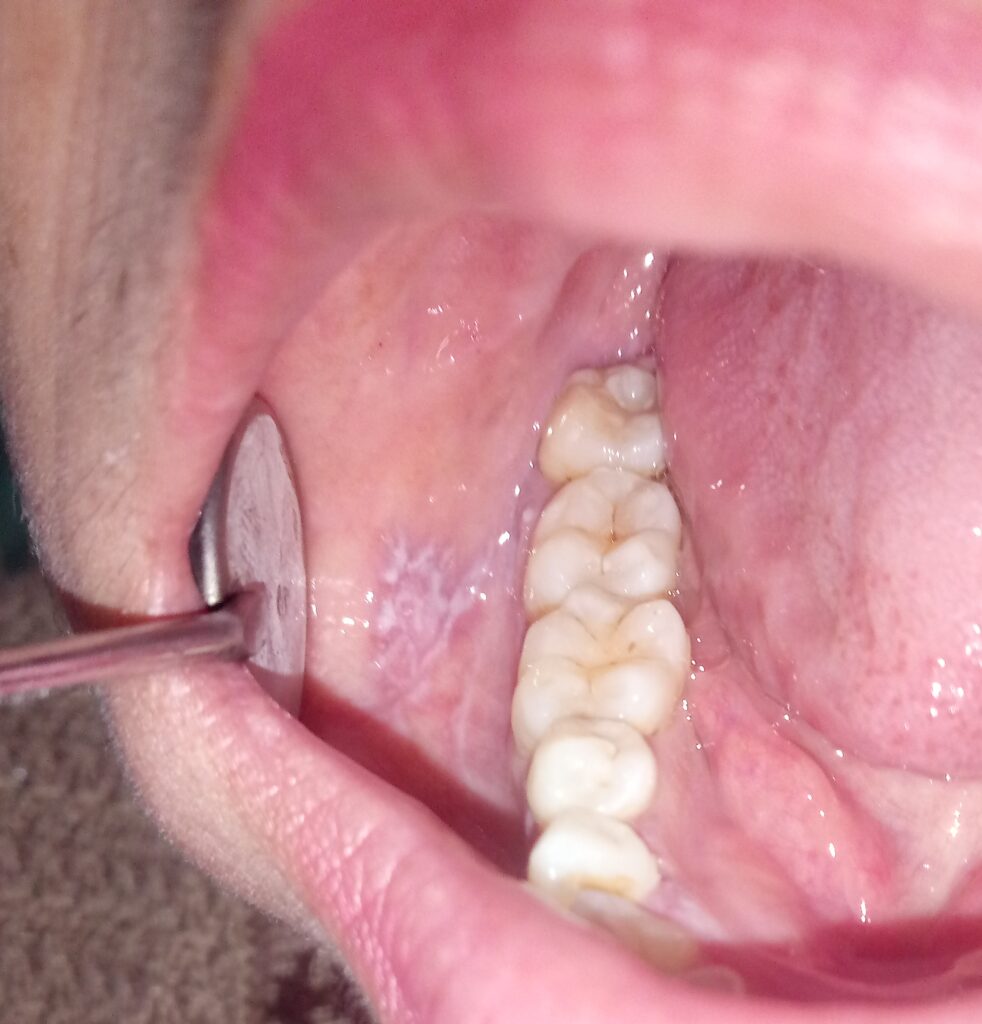
Oral Features of Canker Sores
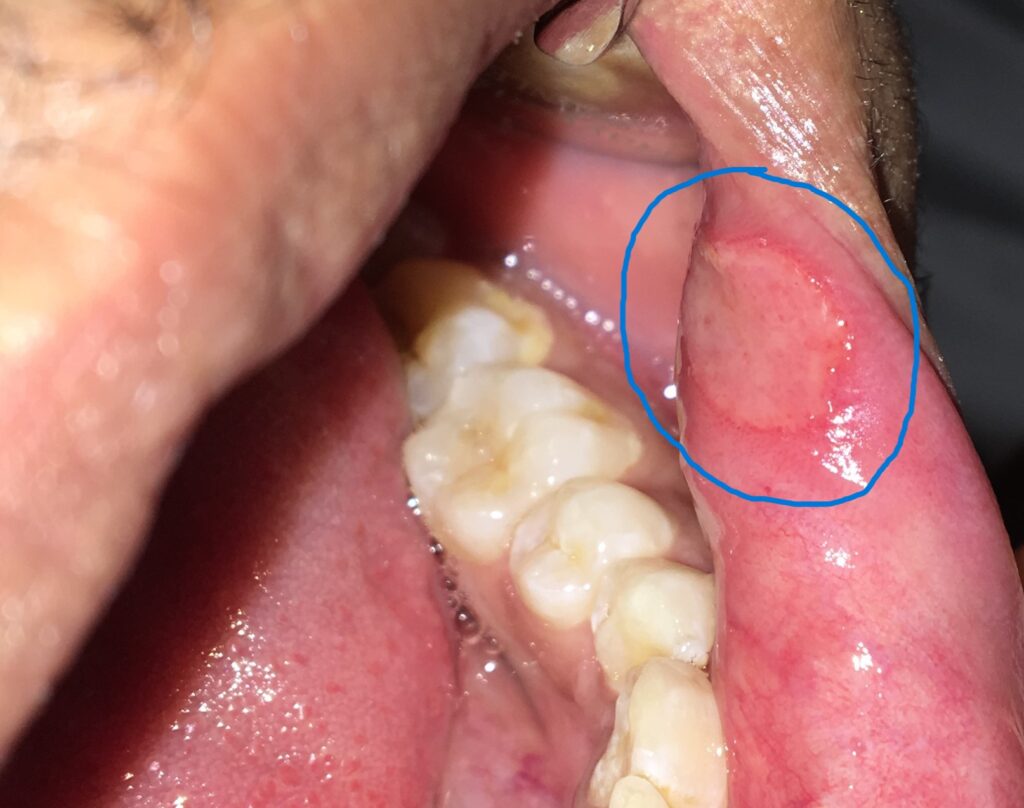
Canker sore
- Usually round or oval, measuring less than 1 cm in diameter.
- Painful and sensitive to touch.
- A white or yellowish base with a surrounding red border.
- Often appear in clusters in severe cases.
- Heal within 1-2 weeks without scarring in most cases.
- Typically occur on mobile (free) mucosa—such as the inner cheeks, lips, tongue, and floor of the mouth—but do not appear on fixed mucosa like the gums and hard palate.
- Tender lymph nodes – In severe or recurrent canker sores, the submandibular lymph nodes may become enlarged and tender due to a reactive inflammatory response. This swelling is usually mild and resolves as the ulcer heals. Persistent or severe lymph node swelling may indicate a secondary infection or an underlying condition requiring further evaluation.
Differential Diagnosis: Conditions That Mimic Canker Sores
Since various oral lesions resemble canker sores, differentiation is important:
- Herpes Simplex Virus (HSV): Contagious, fluid-filled blisters that rupture to form ulcers. Occur on both mobile and fixed mucosa (mucosa that attached to underlying jaw bones) , as well as on the lips and surrounding skin.
- Herpes Zoster (Shingles): Painful vesicles that appear along nerve pathways, affecting both fixed and mobile mucosa. Lesions often form in a dermatomal pattern with a “dew-drop on a rose petal” appearance. It usually affects one side of the face and mouth (unilateral) and rarely occurs on both sides (bilateral).
- ANUG (Acute Necrotizing Ulcerative Gingivitis): Painful gum disease with bad breath and severe inflammation, typically affecting only the gums.
- Erythema Multiforme: Ulcers are deeper, painful, and may cause bloody crusting, especially on the lips. It involves both oral and skin lesions with characteristic bull’s-eye (target) lesions.
If You Experience Recurring Canker Sores, Consult an Oral Physician
While most canker sores resolve on their own, professional evaluation is necessary if:
- The ulcer is unusually large and persistent beyond two weeks.
- Recurrences are frequent and severe.
- Pain is unbearable, affecting eating and speaking.
- There are associated systemic symptoms like fever or diarrhea.
- There is difficulty swallowing or signs of secondary infection.
Investigations When Canker Sores Recur Frequently
- Blood Tests: To check for anemia, nutritional deficiencies, or systemic conditions.
- Allergy Testing: If food triggers are suspected.
- Biopsy: Only recommended when the lesion is persistent, enlarging, or does not heal within the expected time frame. This helps rule out serious conditions like oral cancer or other chronic ulcerative diseases.
Treatment Options for Canker Sores
Treatment focuses on pain relief, faster healing, and preventing recurrence:
Home Remedies
- Saltwater Rinses: Helps reduce inflammation and prevent infection.
- Baking Soda Rinse: Neutralizes acidity and soothes ulcers.
- Honey Application: Known for its antibacterial and healing properties.
Medical Treatments
- Topical Corticosteroids: Such as triamcinolone dental paste to reduce inflammation.
- Antiseptic Mouthwashes: Help prevent bacterial infection in ulcerated areas.
- Pain Relief Gels: Lidocaine-based numbing gels ease discomfort.
- Oral Medications: Severe cases may require systemic treatment like corticosteroids or immunomodulators.
- Laser Therapy: Some dental clinics offer laser treatment for quicker pain relief and healing.
Prevention and Precautionary Measures
- Maintain Good Oral Hygiene: Regular brushing and flossing with a soft-bristled toothbrush.
- Avoid Trigger Foods: Limit acidic, spicy, and hard foods that may irritate oral tissues.
- Manage Stress: Relaxation techniques like meditation may help prevent stress-induced ulcers.
- Correct Nutritional Deficiencies: Ensure adequate intake of vitamins B12, folic acid, zinc, and iron.
- Avoid Trauma to the Mouth: Use orthodontic wax if wearing braces and avoid biting the cheeks or lips.
- Defer Dental Treatments During Active Ulcers: Manipulation of oral tissues during dental procedures can aggravate ulcers and lead to complications like secondary infections.
Role of Oral Physicians in Recurrent Canker Sores
For patients experiencing frequent recurrences, a multidisciplinary approach is necessary:
- Thorough systemic evaluation to rule out underlying conditions like autoimmune diseases or nutritional deficiencies.
- Review of medication history to identify drug-induced ulcers.
- Blood investigations to check for anemia, immune suppression, or systemic inflammation.
- Biopsy if necessary when lesions do not heal, increase in size, or exhibit unusual characteristics.
Conclusion
Canker sores, while generally harmless, can be painful and affect daily activities. Recognizing triggers, maintaining oral hygiene, and seeking timely professional evaluation in recurrent or severe cases can prevent complications. Dentists and oral physicians play a crucial role in diagnosing persistent ulcers and ensuring that no underlying systemic condition is overlooked. Proper treatment and prevention strategies can significantly improve the quality of life for individuals prone to canker sores.
Frequently Asked Questions About Canker Sores
Q: Can stress cause canker sores?
A: Yes, stress is a common trigger for canker sores, as it weakens the immune response and increases susceptibility.
Q: Why do canker sores hurt so much?
A: They expose nerve endings in the oral mucosa, making them highly sensitive to touch, food, and beverages.
Q: Can hormonal changes cause canker sores?
A: Yes, hormonal fluctuations, such as those during menstruation or pregnancy, can contribute to their occurrence.
Q: Is there a genetic link to canker sores?
A: Yes, people with a family history of recurrent canker sores may have a higher risk of developing them.
Q: Can toothpaste cause canker sores?
A: Some toothpaste containing sodium lauryl sulfate (SLS) can irritate the mouth and trigger canker sores in sensitive individuals.
Q: Can dehydration worsen canker sores?
A: Yes, dehydration can dry out the oral mucosa, making it more prone to irritation and delayed healing.
Q: Do canker sores always heal on their own?
A: Most heal within 1-2 weeks, but larger or persistent sores may require medical treatment.
Q: Can vitamin deficiencies cause canker sores?
A: Yes, deficiencies in vitamin B12, iron, folic acid, or zinc can increase the likelihood of developing canker sores.
Q: Why do canker sores sometimes occur after dental work?
A: Trauma from dental procedures, sharp edges, or ill-fitting prosthetics can trigger canker sores.
Q: Can spicy food make canker sores worse?
A: Yes, spicy, acidic, or rough-textured foods can irritate sores and prolong healing.
Q: Is it normal for canker sores to cause mild fever?
A: While uncommon, severe cases may trigger a mild fever due to the body’s inflammatory response.
Q: Can probiotics help prevent canker sores?
A: Some studies suggest that probiotics may improve oral health and reduce the frequency of canker sores.
Q: Do canker sores indicate a weak immune system?
A: Frequent or severe canker sores can be a sign of an underlying immune system issue that should be evaluated.
Q: Can mouthwash help with canker sores?
A: Alcohol-free, antiseptic mouthwashes can help reduce bacteria and promote healing, but strong, alcohol-based rinses may worsen irritation.
Q: Do canker sores spread in the mouth?
A: No, they do not spread like infections, but multiple sores can appear simultaneously, especially in severe cases.
Q: Can smoking cause canker sores?
A: Smoking irritates the oral mucosa and can increase the risk of canker sores in some individuals.
Q: Can allergies cause canker sores?
A: Yes, some food allergies or sensitivities may contribute to recurring canker sores.
Q: Do canker sores leave scars?
A: Small canker sores usually heal without scarring, but large or deep ulcers may leave slight scarring.